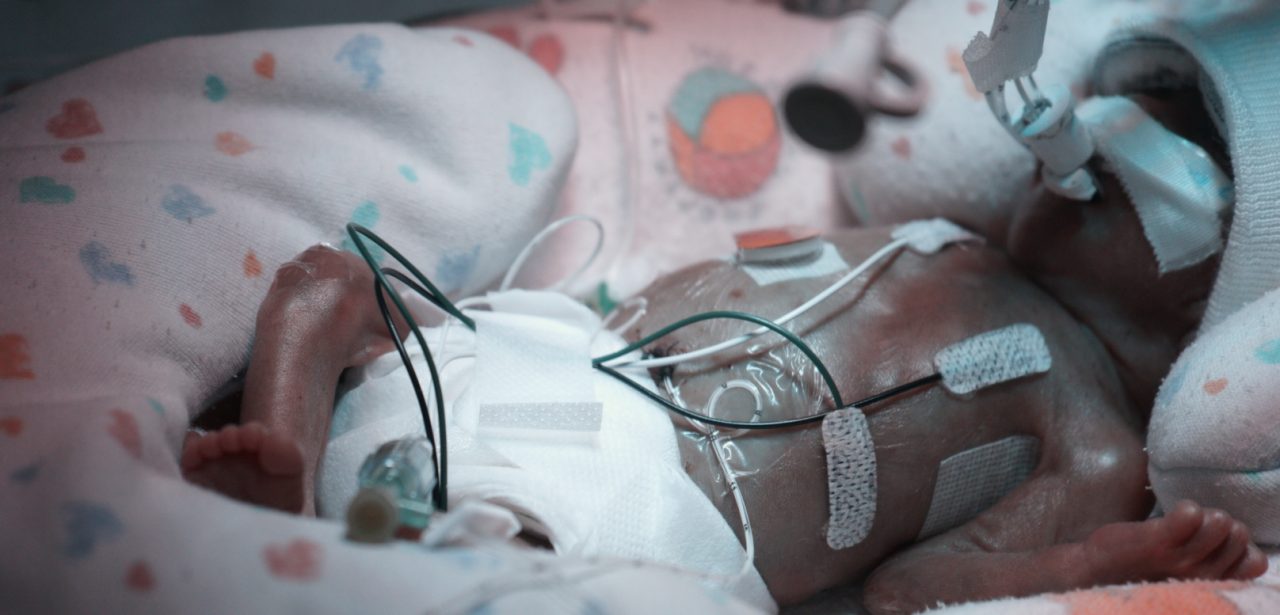
Came in and he was on 26% oxygen.
A nurse we have never had before in 115 days of life.
She has had a good morning so far.
Said she pointed out when assignments were made that she had never had him. She asked for tips or recommendations, I said, just keep doing what your doing if you’ve had a good day.
Cares. Just pee.
Lunch.
Back up to NICU.
Dr. Comes by, good talk about everything. He is working on a passdown to PICU for when the time comes. He shows us RT’s growth chart, he is close to the fifty percentile, impressive considering everything he has been through and the steroids he is on that stunt growth.
Cares, skin to skin. Takes a long time to settle, might be because the way the et tube lock is taped its close to his eye when he lays on this side.
23% through all of skin to skin.
3 hours later, skin to skin time is up.
Put him back, cares.
26% oxygen.
Dinner.
Back to NICU.
27% oxygen. Another nurse that has not had him…. bummer.
Blood gas before cares. Good blood gas, better than he has had in a while!
Nurse gives him his meds. She starts to put some into his mouth. I ask what she is putting in his mouth, she stops. Says it’s the anti gas medication. I tell her no one, has ever put medication in his mouth not sure what she is doing.
He has a ND tube for a reason. She says it works better if it’s given orally, and the morphine has a bubble gum taste.
Wait so she was going to give him his morphine orally too? They have always given him his meds into his ND. We don’t even know if he can swallow. He has not ever been been fed orallu. Plus if the fluid follows the ET tube it will go into his lungs… so he could get pneumonia.
Wonder what happens if he aspirated simethicone.
Simethicone is an anti-foaming agent that decreases the surface tension of gasbubbles, causing them to combine into larger bubbles in the stomach that can be passed more easily. Simethicone does not reduce or prevent the formation of gas in the digestive tract; rather, it increases the rate at which it exits the body
Cares, change his diaper, just pee. Spo2 is 95. Go to wash my hands. Spo2 is down to 33… what happened!?
Respiratory therapist Neopuffs him.
Confused as to what happened. He got down to 54 before the monitor even alarmed.slight brady.
He comes back up. No one really knows what happened.
They listen to him with a stethoscope, sounds diminished in upper right lobe.
Maybe he did aspirate some of the medication put in his mouth. We have seen reactions like that when he got rainout.
We finish cares and reposition him on his left side. He looks relaxed.
I wait for night rounds and ask for an xray because we haven’t had one in a while yet have been changing many things. We DC zopanex, Hypertonic saline, and cpt and still haven’t gotten one in a while. While I underarms clinically he looks like he does not need one. In the past he did not look like he needed one either. He sounds diminished in upper right lobe. I have a discussion with the doctor for about 10 minutes.
He feels RT is looking excellent from a clinical stand point. Lower support than we have had in a while, good blood gas, lower oxygen needs.
While I agree he looks good he has done this in the past, then one small event hapens and we get told that he just had no reserve and it tipped him over the edge.
Even when we got intubated this time, his blood gas looked good, his oxygen needs were low 21% at intubation. But he was having more frequent deeper events.
Doctor feels an x-ray would be unnecessarily exposing him to radiation. He feels they would not gain any knowledge from it.
I understand but disagree.
Doctor would rather get one tomorrow after switching to NAVA I mode of ventilation.
I point out if we get one after switching if we see worsening we would assume it’s because we switched to NAVA not because we DC his medications several days ago.
His leak around his ET tube is bigger on his left side. He desats. Turned up to 33%. Higher than he had been all day, maybe just because his leak is big. Who knows. Maybe it’s because he inhaled medication someone put in his mouth…
I guess we will find out tomorrow.
Hang out, tell RT goodnight.
Difficult to leave but he is comfy looking and mostly asleep. Hopefully just his leak causing the higher oxygen. If we have higher needs tomorrow that started tonight we will know why.
I call the NUCU when I get home and talk to our nurse again about not putting medication in his mouth, we don’t need him inhaling morphine too, she won’t do it again and will pass it on. She is nice and thanks me for calling.
Sleep tight not so tiny boy!