0600 wife wakes me up. It’s time to get ready to go up to the NICU.
After getting ready, we head up. We arrive at the NICU around 630.
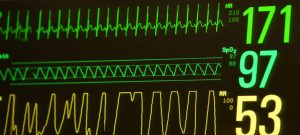
Nurse tells us she was just getting ready to call us. RT had one big de-sat over the night, and many smaller ones. A new blood gas, does not look good. Almost all the settings are turned up on the ventilator to try and improve it. She shows us a new xray, maybe it looks slightly better.
This is the first time this nurse had him, she seems to have bonded with him over the night.
Oncoming nurse is one of the nurses that kindly volunteered to be more primary care for him.
Talking about weaning him on vent settings because xray looks slightly better. It is still horrible.
Dr. has concern that RT is over diuresed and becoming dehydrated, he thinks this is causing his increased oxygen needs and his heart rate to increase.
This is one symptom of dehydration adults have that babies may also have. Labs ordered to confirm, waiting on results.
I feel he isn’t basing his actions on actual numbers, labs or facts, reaching for ways to try and help without good direction before labs are done.
Perhaps this is because I like percents numbers pictures and more tangible evidence.
Then again, preemies are not helicopters.
Sometimes doctors have to act fast before having all the numbers.
Dr. has D/C’d lasics so that RT won’t be getting rid of as much fluid.
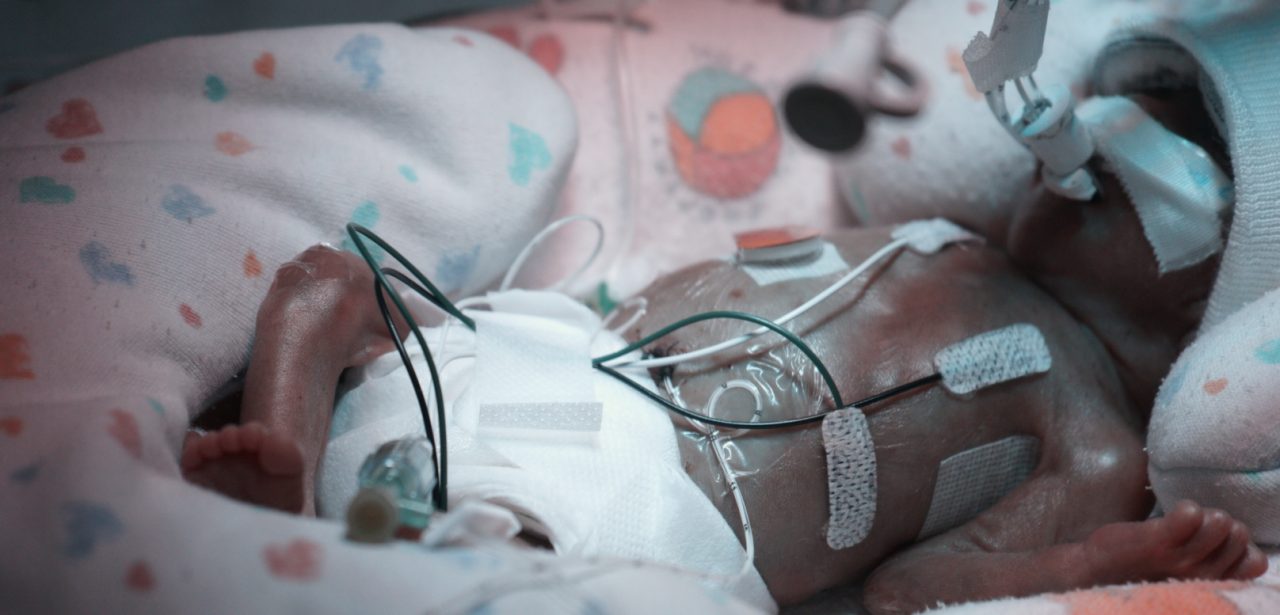
0712 comes, RT is now one month old! Happy birthday! Gestation would be 28 2/7. We tell him happy birthday, and give him some hand hugs. I’m proud of him for making it through another tough night.
Time to go get breakfast.
I am burnt out, I take a nap. Mom takes care of some chores for us and heads back up to NICU.
New Dr. comes onto shift.
New Dr. Wants to make some more changes, labs are back.
1130 wife let’s me know, I head back up to NICU.
1145 I’m at NICU again, wife is sitting bedside talking with the Dr.
Labs are back, RT is not dehydrated.
Another set ordered for noon
The Dr. tells us the plan moving forwards. She thinks we need to try a different ventilator called an oscillator. She believes it will help re-inflate his little lungs.
An oscillator essentially keeps a constant pressure on lungs while cycling the air, rather than normal breaths with peaks and valleys of pressure.
Some Drs believe it is a step backward, other Drs believe it is another useful tool, not a step backwards, but a better way to allow his lungs to heal without having to deflate and reinflate each breath like a sticky balloon trying to be inflated the first time.
We start preperations, move chairs out of the way, and re-arrange furniture.
They bring in the oscillator.
It is old school. A big clunky box on wheels with hoses, wires, and alarm clock red light up numbers.
If this helps I’m all for using different tools for different purposes.
They hook it up and begin the transition. They turn it on, it sounds like an air pump. They quickly swap connections over and RT is now on an oscillator, they adjust some settings.
The Dr. observes the transition and recommends some settings changes.
She says he isn’t shaking enough.
I guess this is one of the circumstances it is ok to shake babies.
They adjust it some and then his little body shakes as the pressure oscillates quickly. He seems a bit agitated by the new machines sounds, being moved to accommodate the stiffer tubes, and the shaking. He slowly calms down.
They begin to slowly wean his oxygen percent.
X-ray arrives too quickly. It was ordered of one hour after swapping to the new system. He is told to come back.
Time for mom to pump. The new loud machine and stress don’t seem conducive to pumping.
Xray comes back when it is time. They take an image, the Dr comes and looks. Has it sent to her computer and calls us into her office to look at new xray and previous one.
There seems to already be better lung recruitment, but still a ways to go. We have a good talk with the Dr. about different perceptions about the machine and why it is a better tool for doing what we need.
The plan moving forward is to continue with this vent for several days then potentially back to NAVA ventilator to see if he can breath on his own once his lungs are inflated. Then if that works on to NIV NAVA.
It’s already been a long day for little RT. He continues to fight on.
Dinner time. Grab some things from hotel. Eat some food.
We have a parent sleep room tonight and tomorrow to be closer to RT. He will be sleeping 4 floors above us.
Back to NICU. His blood gas numbers are looking better than this mornings.
He is still requiring 67% oxygen. Hopefully as his lungs expand needs will diminish. They continue to get large clots and blood from lungs at care times. Occasionally it is only white thick secretions.
Tonight is another nurse that volunteered to be his continuity of care which we are grate full for.
While preemies are on the oscillator they require a designated nurse that only works with them.
It’s been several days since we have seen her, with many changes.
Shift change happens, the nurses do the pass down, then we tell her the stories of the last couple days.
Time for cares, mom cleans his eyes, I clean his butt. Just pee this time. He pees again just as I’m about to finish! Good job RT!
We get to swap out RT’s incubator back to the giraffe version which is more designated for micro preemies. I think it is slightly nicer. I have the pleasure of holding him during the transfer. It goes fairly smoothly but he is agitated from the movement once we get him in the new bed.
Oxygen needs are close to 100% temporarily.
It’s time to let him rest recuperate and recruit his lungs.
Thank you nurses and Drs, we are grateful for you.
Another day tomorrow.
Praying for no phone calls.
Sleep sweet RT, we are just downstairs tonight.